Management of deep splitting root canals
24/07/2023
Fellow
Warning: Undefined variable $post in /home/styleendo/htdocs/styleitaliano-endodontics.org/wp-content/plugins/oxygen/component-framework/components/classes/code-block.class.php(133) : eval()'d code on line 2
Warning: Attempt to read property "ID" on null in /home/styleendo/htdocs/styleitaliano-endodontics.org/wp-content/plugins/oxygen/component-framework/components/classes/code-block.class.php(133) : eval()'d code on line 2
Endodontic management of a tooth is an interesting and challenging procedure that is partly blinded, and its success depends on individual clinical expertise and skill, as well as the procedural techniques applied.
Tooth anatomy is the map on which every clinician relies upon prior to initiating root canal treatment.
The vast data on tooth anatomy available to the scientific community does allow for a better understanding of the tooth’s internal anatomy and its numerous variations.
Mandibular premolars have known to be the most challenging teeth to be treated endodontically, especially when they present with multiple roots or canals as they are known to have numerous anatomic variations of their roots and root canals, which are a challenge to treat efficiently.
In the simplest form, each root has a single canal and a single apical foramen. Commonly, however, other canal complexities are present and exit the root as one, two, or more apical canals.
This could be better understood through an insight into the development of root formation. At a more advanced stage of tooth development, when enamel and dentin formation has reached the future cementoenamel junction, the dental root begins to form from a cellular diaphragm or horizontal Hertwig’s epithelial root sheath. The horizontal Hertwig’s epithelial root sheath may vary in shape, depending on whether the teeth are single or multi-rooted. In fact, its shape determines the number of roots in a tooth. If the diaphragm remains in the shape of a collar, a single- rooted tooth will form. On the other hand, if two or three tongues of epithelium grow towards each other from this collar to bridge the gap and fuse, two or three diaphragms evolving independently from each other will form. They will either remain fused, forming fused roots, or single roots with multiple canals, or separated, forming distinct roots in multirooted teeth.
The purpose of this article is to outline relevant documented clinical methods and techniques that would be beneficial to successfully negotiate various anatomic aberrations specific to mandibular premolars.
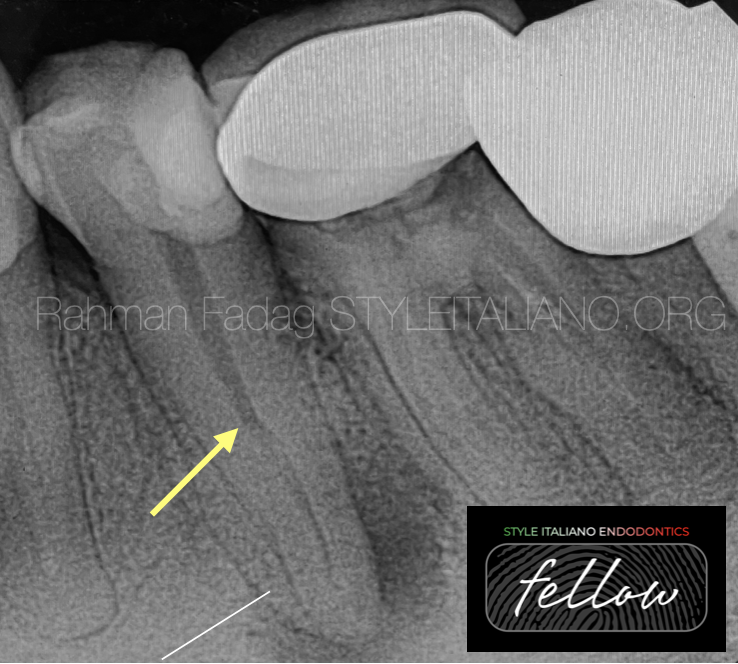
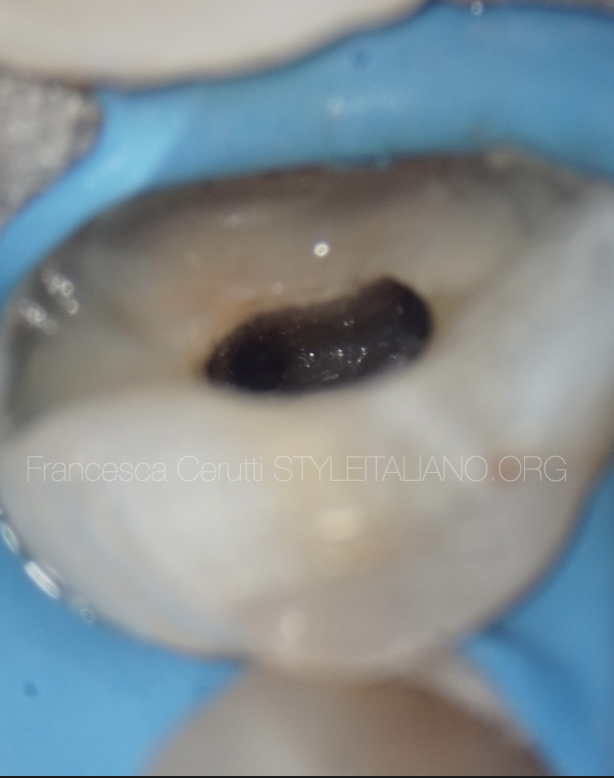
Fig. 1
A sudden change in radiographic density of the root canal space usually indicates an additional canal or a canal bifurcation.
If a radiograph shows a sudden narrowing or even a disappearing pulp space, the canal diverges at that point into two parts (yellow arrow).
Wide apical part of the root rather than narrow indicate bifurcation or even trifurcation (white line).
Radiographic interpretation of some accessory roots and their root apices may be difficult due to:
- Their close proximity to each other.
- There exists a possibility of superimposition by other roots.
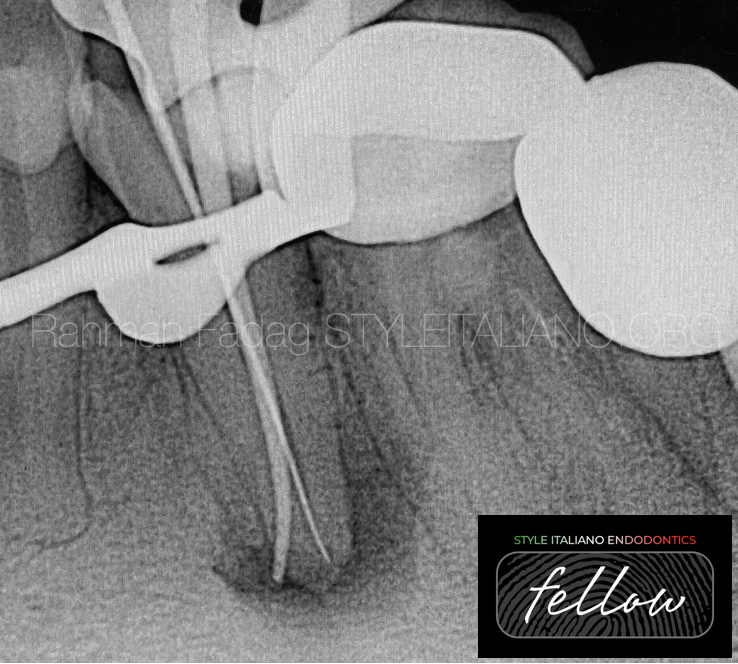
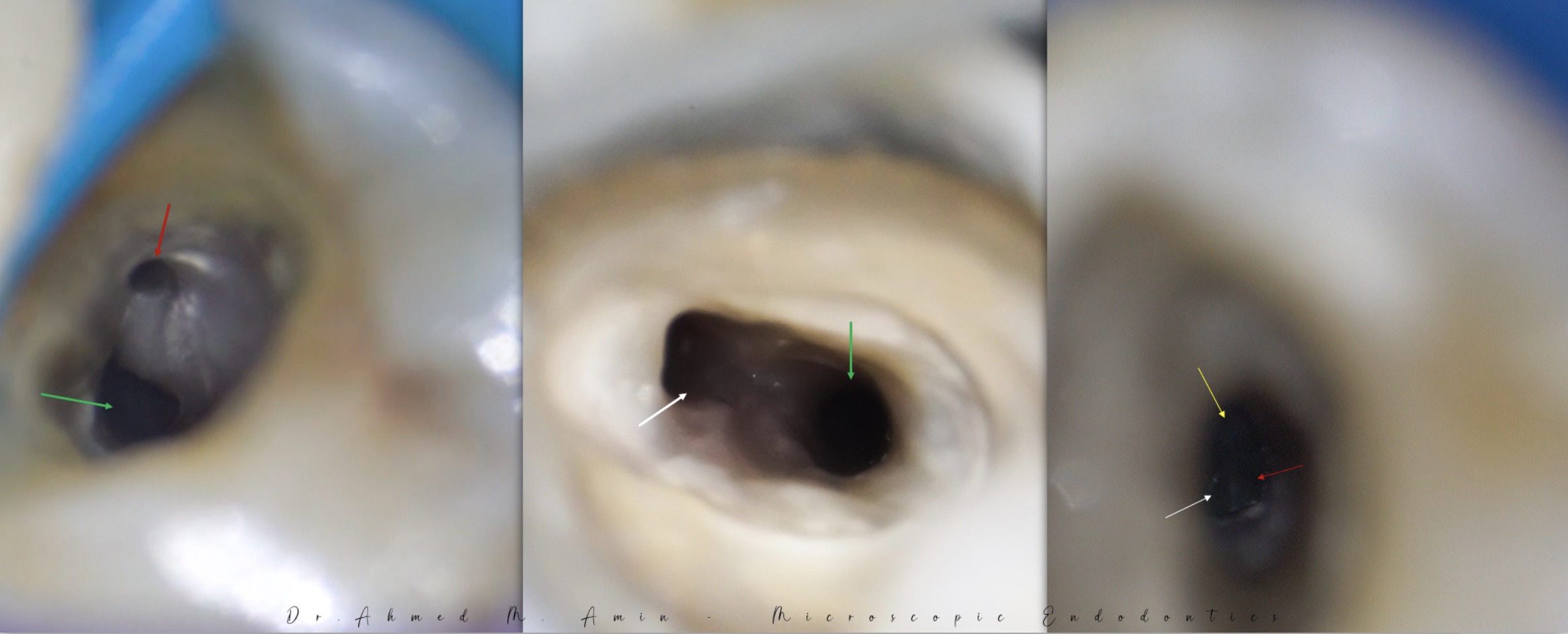
Fig. 2
An apex locator is very useful in such cases and can be used to estimate the root canal lengths prior to a confirmatory working length radiograph.
If a working length file appears off-centre on the radiograph, multiple canals should be suspected.
It’s better to conform the working length by inserting gutta-percha point in one canal and a file in the second one because of the difficulty in putting two gutta-percha points in the narrow space.
One should remember the following:
1- presence of a sharp curve especially in the bifurcation or trifurcation area.
2- dentin thickness in multiple canals premolars.
3- Any incidence of file separation within the complex canal system makes retrieval extremely difficult and also renders the root walls highly susceptible to perforations.
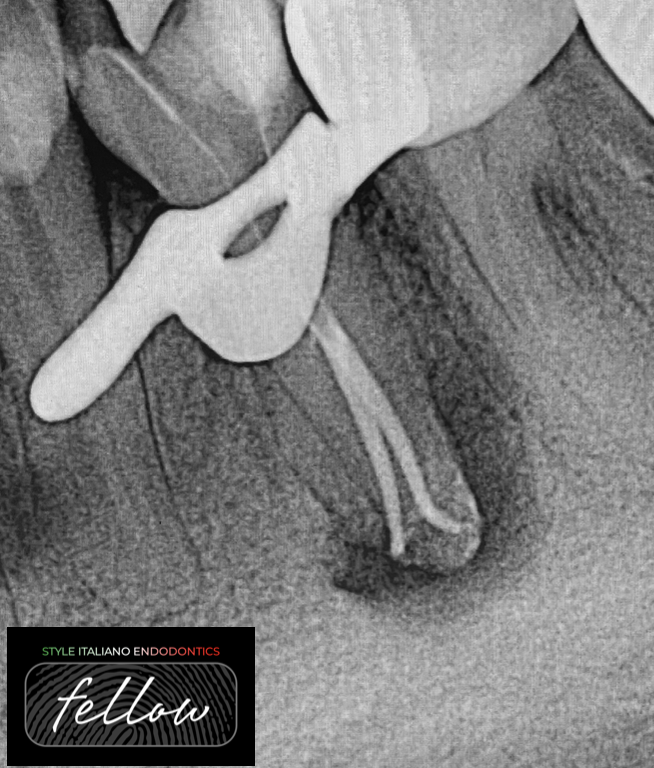
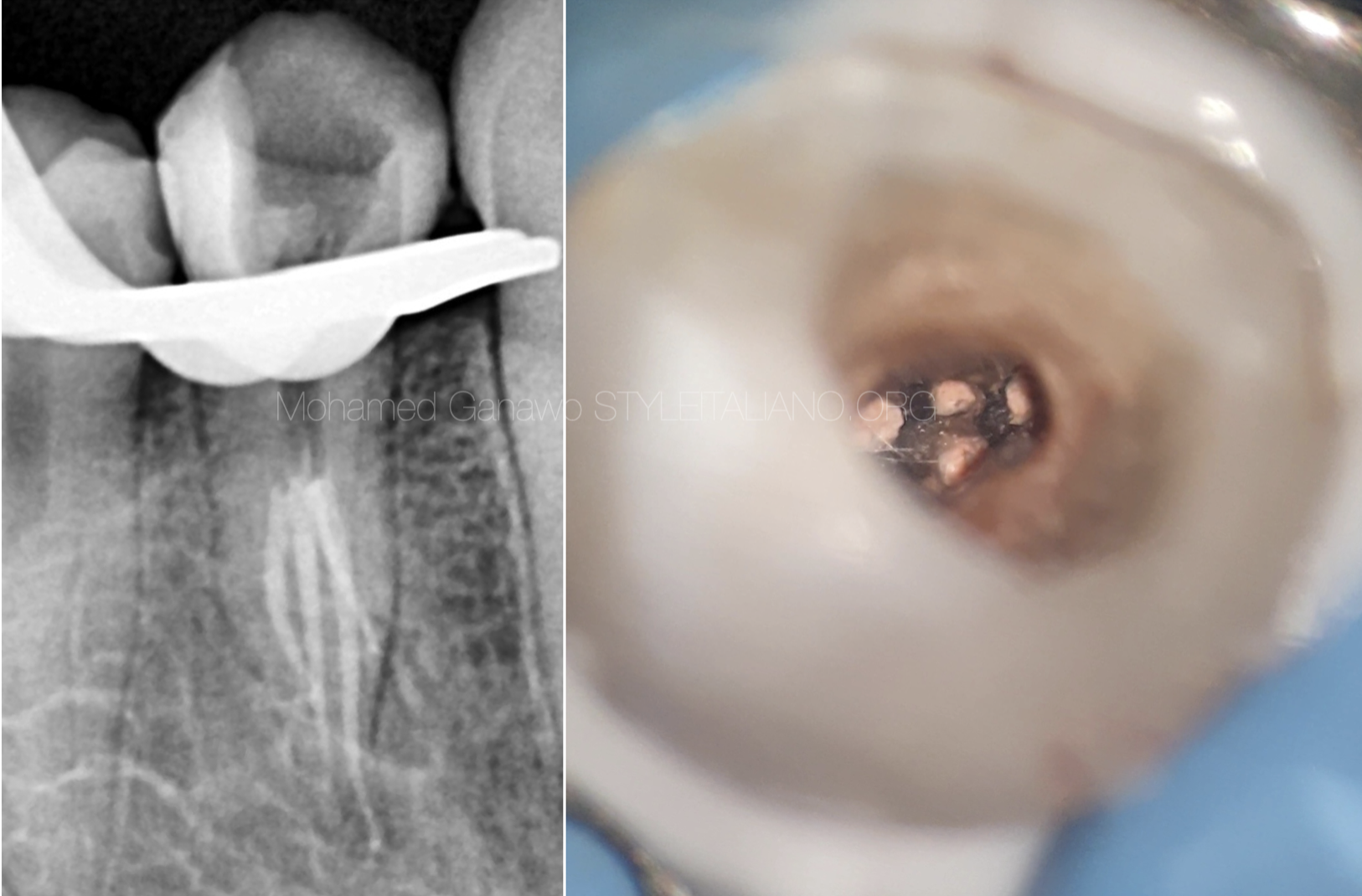
Fig. 3
The pulp space of mandibular premolars commonly contains isthmuses, lateral canals, apical ramifications and other irregularities. The use of adjuncts to cleaning and shaping in the form of passive ultrasonic irrigation, apical negative pressure irrigation devices, or other dynamic modes of irrigation could be useful in enhancing disinfection and cleaning the uninstrumented apical bi- and trifurcations and lateral ramifications that are the most difficult to instrument. The use of an irrigation needle with a smaller diameter could result in enhanced irrigant flow into root canal irregularities.
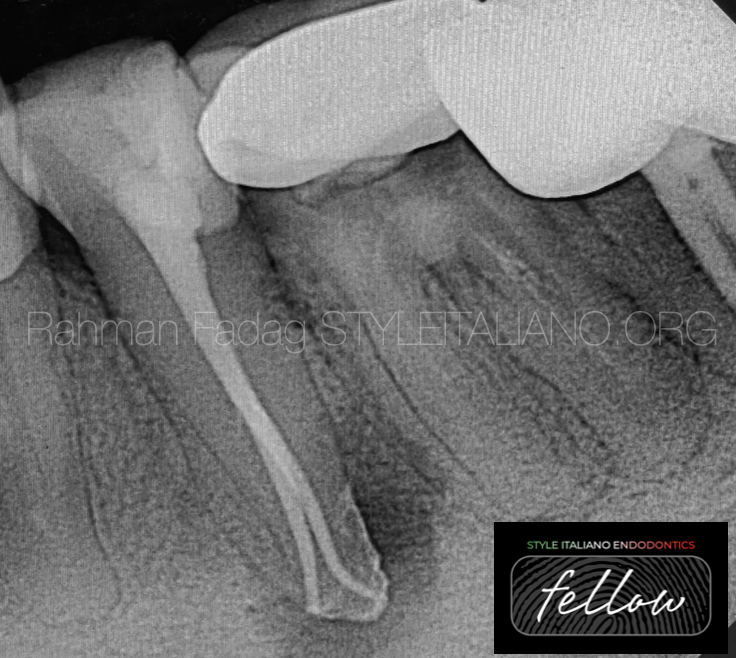
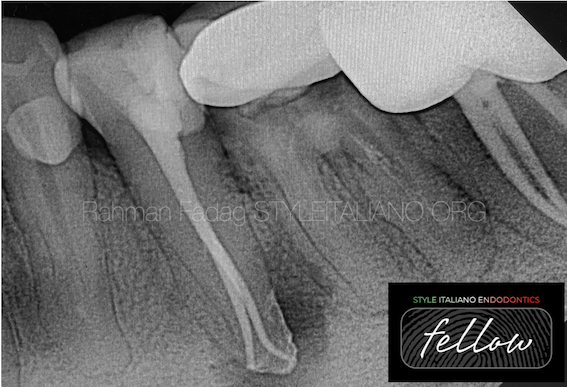
Fig. 4
Obturating such root canal systems requires good clinical skill along with a dental operating microscope with higher depth of focus.
Warm obturation techniques are the best choice to fill such anatomy.
Squirt technique.
In this technique, both ends of the root canals are obturated simultaneously by injection of thermoplasticized gutta percha, followed by back filling.
Alternately, two or three separate master cones are used with each cone being sheared apical to the bi- or trifurcation.
Obturation systems can be used efficiently to fill such canal configuration.
Conclusions
Clinicians undertaking treatment of such complex anatomy cases need to be extremely patient as prolonged and multiple appointments are very much a certainty.
The time involved in treating such complex cases of variable tooth anatomy is mainly dependent on the clinical skill, expertise, and proficiency of the endodontist and the armamentarium available to achieve optimum clinical outcome.
Practitioners who regularly treat different population origins should be aware of racial differences and their influence on pulp space anatomy.
To ensure endodontic success we should consider the vital role of the following:
- Thorough understanding of normal anatomy and common variations.
- careful interpretation of angled radiographs
- use of three-dimensional imaging (CBCT).
- proper access cavity preparation.
- detailed exploration of the interior of the tooth, ideally under magnification.
Bibliography
1- H. Yang et al. “A cone-beam computed tomography study of the root canal morphology of mandibular first premolars and the location of root canal orifices.,” Journal of Endodontics, 2013.
2- M. Lipski, “Root surface temperature rises during root canal obturation, in vitro, by the continuous wave of condensation technique using System B HeatSource,Endodontology, 2005.
3- D. da Silva, U. Endal, “A comparative study of lateral condensation, heat-softened gutta-percha, and a modified master cone heatsoftened backfilling technique,” International Endodontic Journal, 2002.