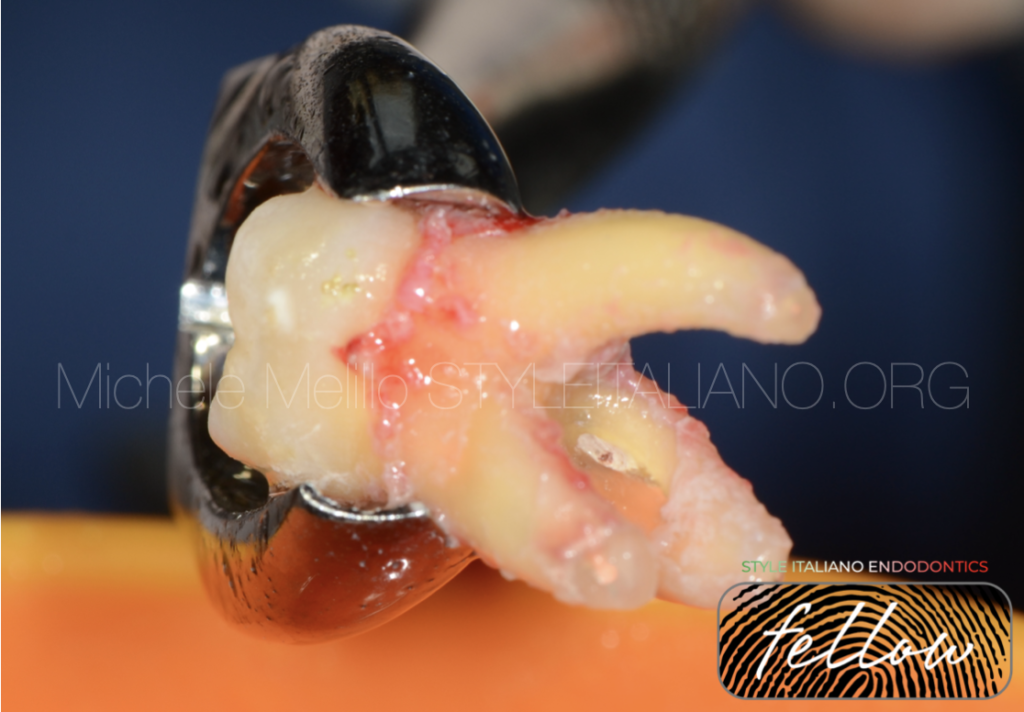
Tooth Autoreplantation of 1.6 with stripping
30/03/2025
Fellow
Warning: Undefined variable $post in /home/styleendo/htdocs/styleitaliano-endodontics.org/wp-content/plugins/oxygen/component-framework/components/classes/code-block.class.php(133) : eval()'d code on line 2
Warning: Attempt to read property "ID" on null in /home/styleendo/htdocs/styleitaliano-endodontics.org/wp-content/plugins/oxygen/component-framework/components/classes/code-block.class.php(133) : eval()'d code on line 2
The patient arrived with an acute lesion on the vestibular area of the tooth 1.6. Also probing was present on the vestibular furcation. After a cbct examination a missed MB canal was found and on the MB2 it was clear the presence of a stripping lesion .
Our first choice was the RCT of the tooth. The Mb canal was found and treated and also the MB2, D and P canals were retreated. During the tridimensional obturation of the MB2 the stripping was directly approached with bioceramic putty.
After 1 month the patient come for the monthly recall but the fistula was still present and pain was also referred.
Oure second choice was a surgical approach for a direct restoration of the root.
On the 3d exam was well represented the lesion but the vestibular cortical bone was well preserved. So to reach the lesion we had to check if we had enough space to clean and seal the root.
This video shows the base line. Before the RCT of the tooth 1.6.
We can appreciate the lesion on the vestibular furcation,
The missed MB canal, the stripping at the middle third on the MB2 canal and how difficult was the anatomical access at the lesion for a direct restoration.
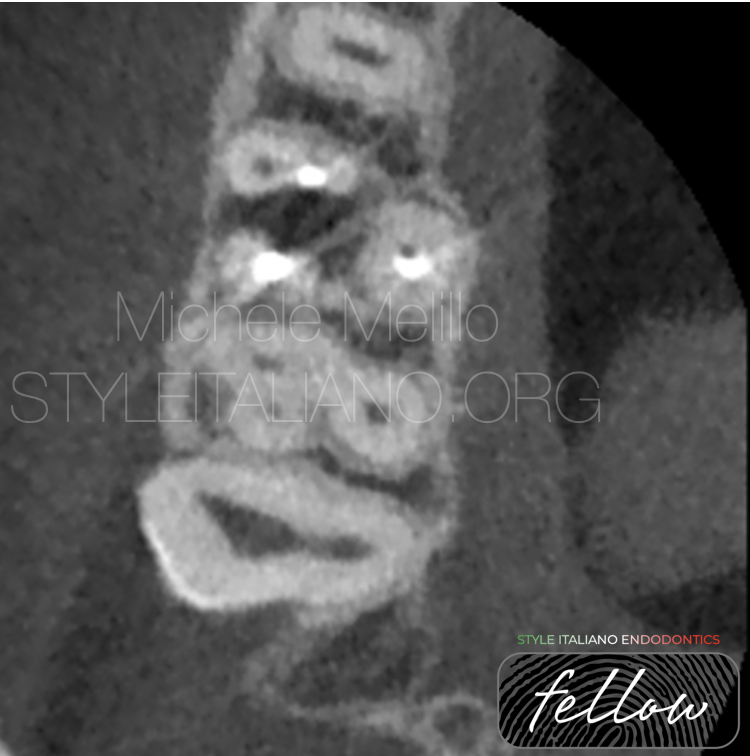
Fig. 1
The anatomy of the MB root made the vestibular space too tight to reach the inner part of the root and to allow a good visibility to clean, prepare and restore the lesion
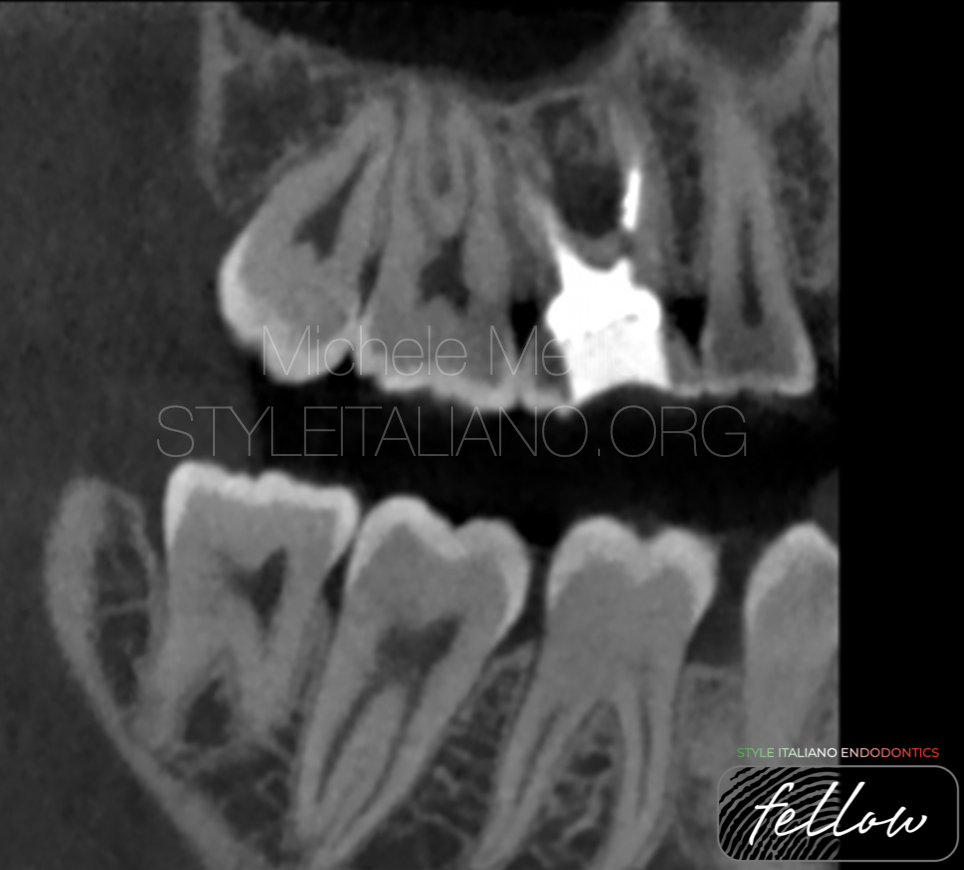
Fig. 2
A section one the Mb2 canal shows the stripping and the extension of the lesion at the furcation.
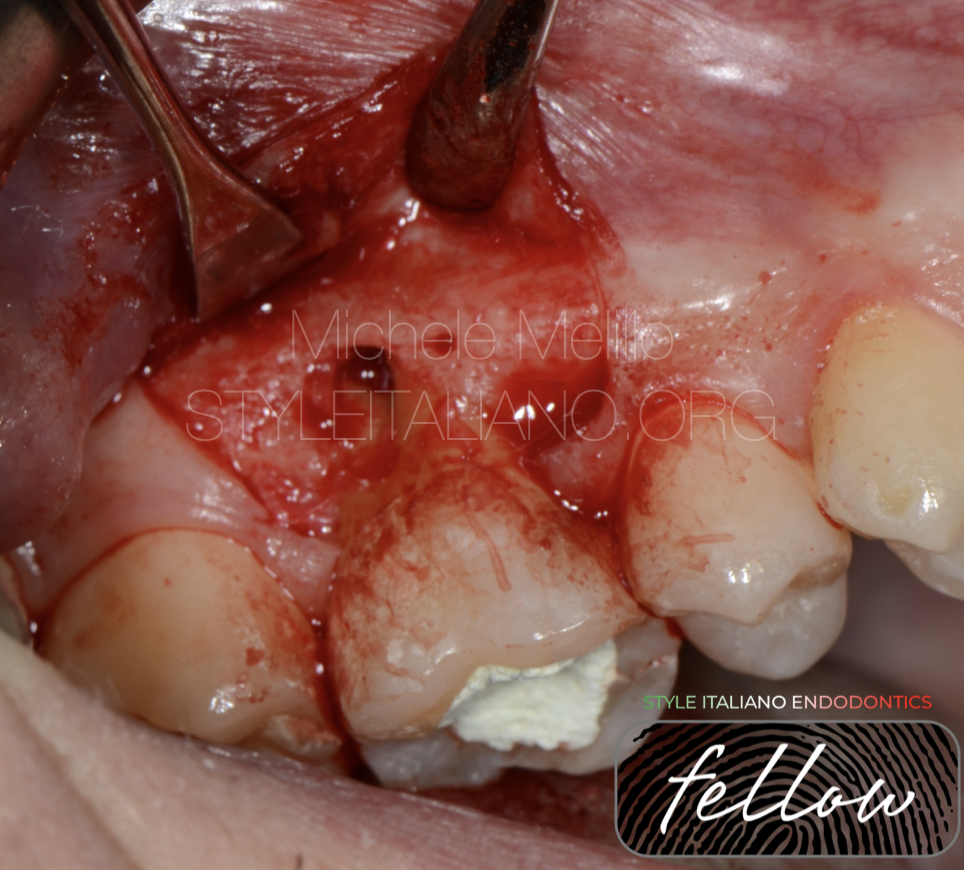
Fig. 3
After the elevation of a mucoperiosteal flap we were able to better confirm how the anatomy made impossible a direct approach to the lesion. It was need a huge osteotomy to increase the space and visibility and this option was discarded to preserve the bone for an implant in case of failure in the future.

Fig. 4
So our best option has been the tooth extraction to try the resolution of the problem in a easier way extra orally.
A very gentle explantation was performed with forceps due to preserve the periodontal ligament vitality.
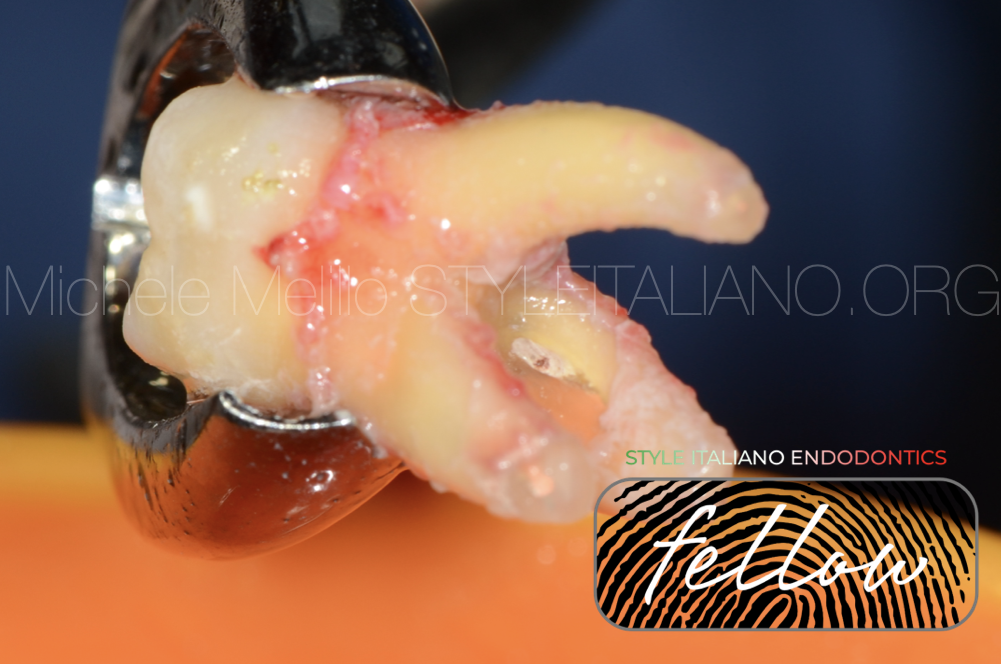
Fig. 5
After removing the granulation tissue from the root, the extent of the stripping lesion was clearly visible.
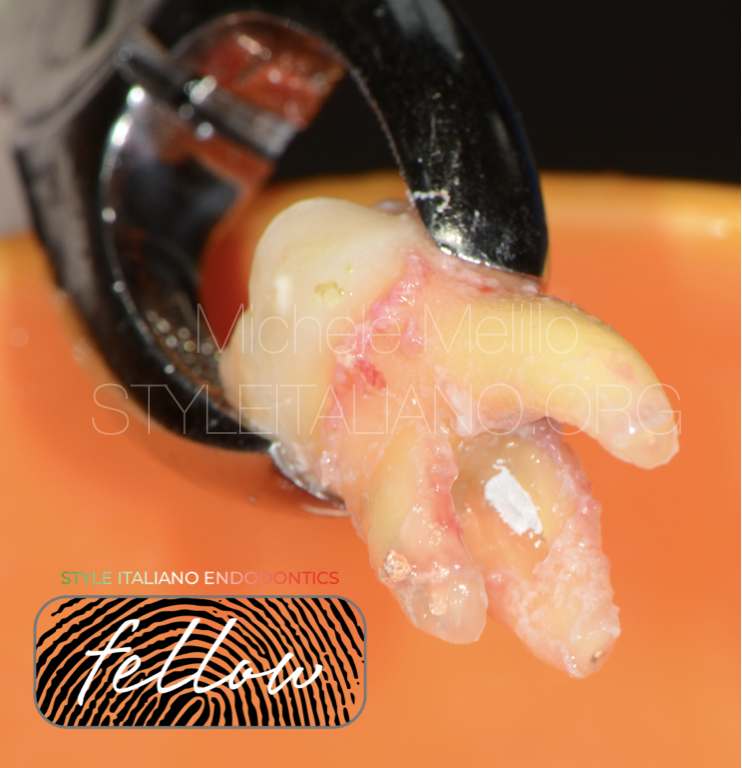
Fig. 6
The lesion was cleaned with burs, at low speed and rinsing with physiological solution.
Than the root was restored with a bioceramic putty (Well Root, Dental World) that allows a fast setting to reduce the total extra oral time (less than 15 min).
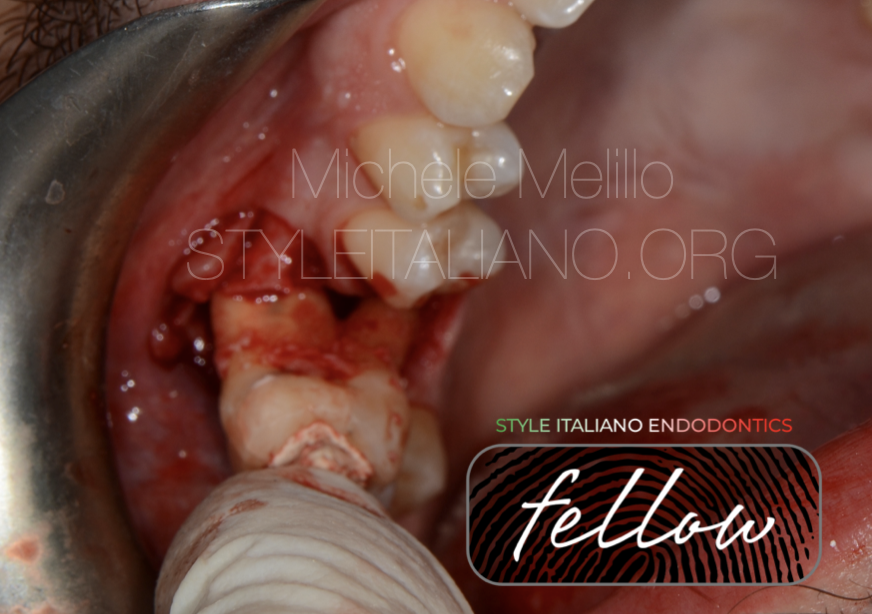
Fig. 7
The tooth was placed back into its socket.
Due to the divergent root anatomy an alveolar expansion with osteotomes was needed to allow the positioning of the tooth friction free.
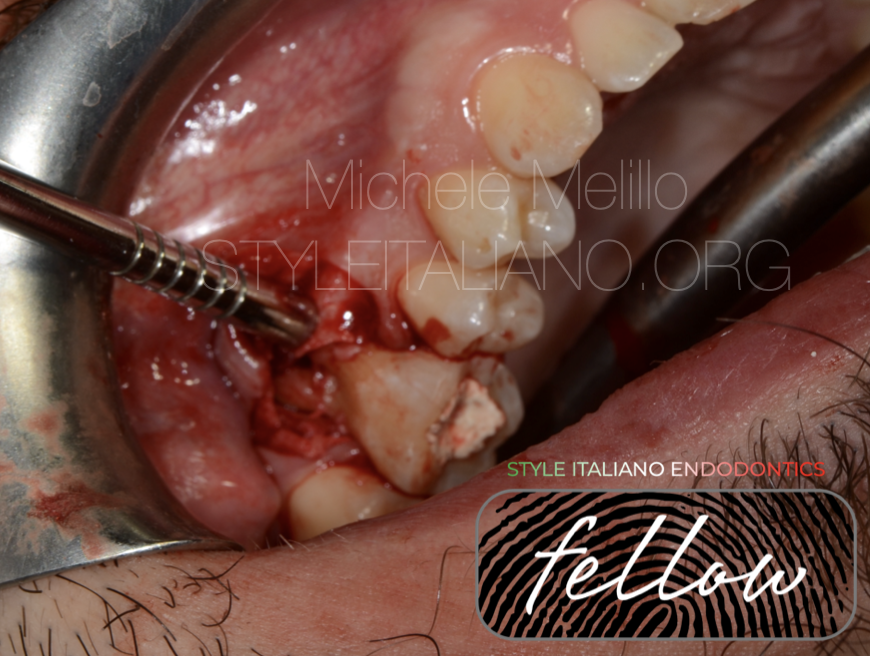
Fig. 8
After checking that the original position was obtained, the vestibular bone was adapted on the root with osteotomes to reduce the gap between roots and bone.
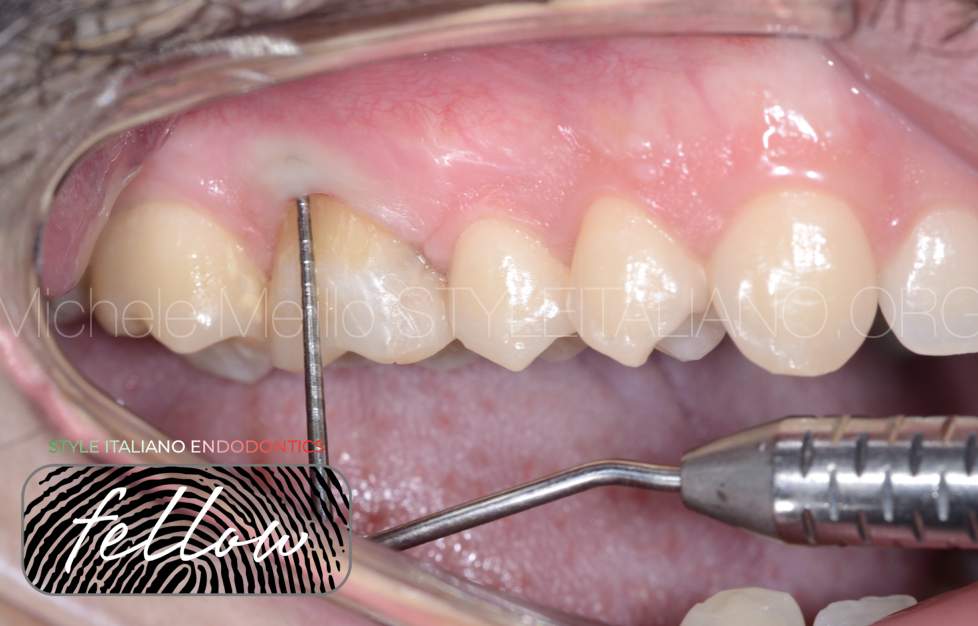
Fig. 9
At the tree months recall the tooth was healthy, no probing or bleeding on probing.
No mobility and at the percussion the sound was physiologic (metallic sound is sign of ankylosis).
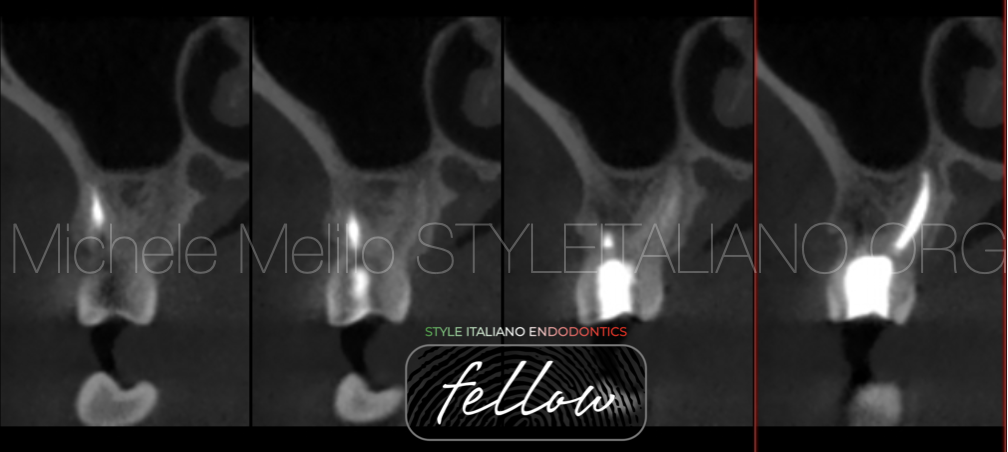
Fig. 10
At 1 year recall we decided to investigate the healing with a low dose CBCT.
At the cross sections we can appreciate the complete healing with the new bone formation and the complete healing of the furcation lesion.
The Buccal bone is remineralized and no signs of periodontal lesion.
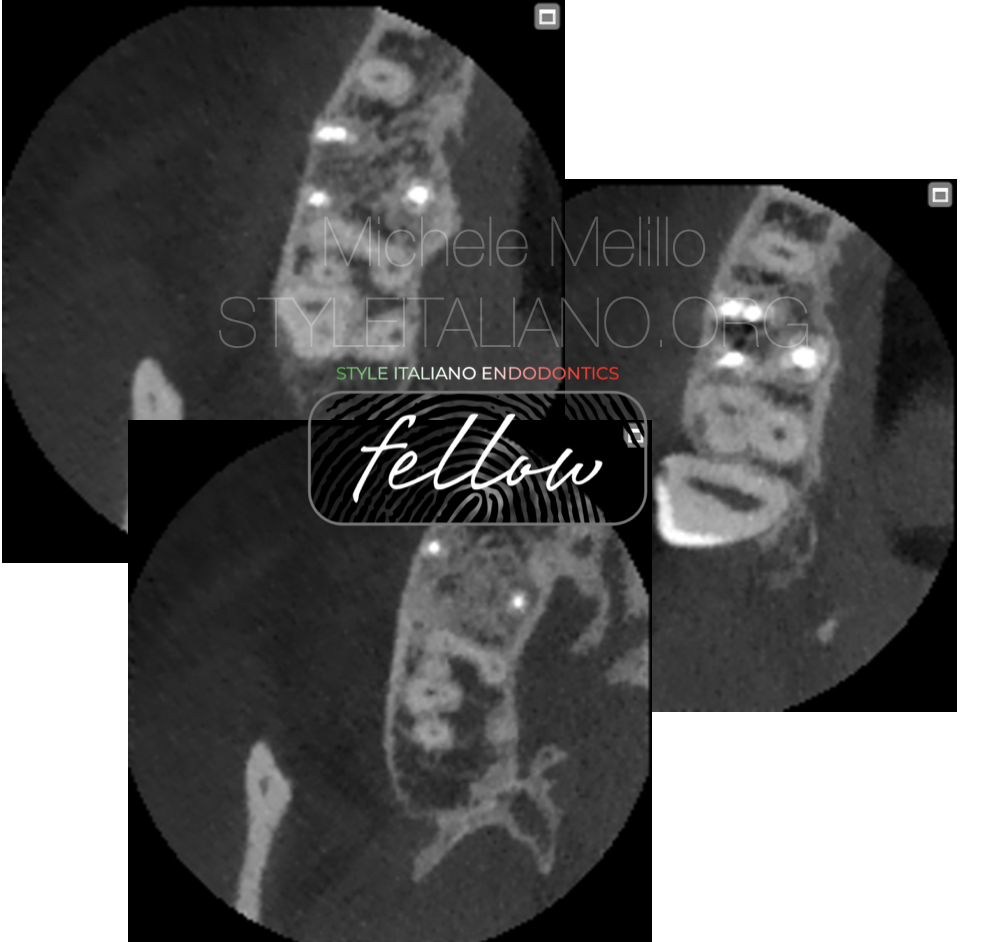
Fig. 11
On the axial view we can appreciate the mineralization of the buccal bone and the the filling material that completely seal all the 4 canals.
The furcation defect si completely healed due to the periodontal ligament’s power.
In this video you can explore different section that confirm the complete healing 1 year post the intentional replantation.
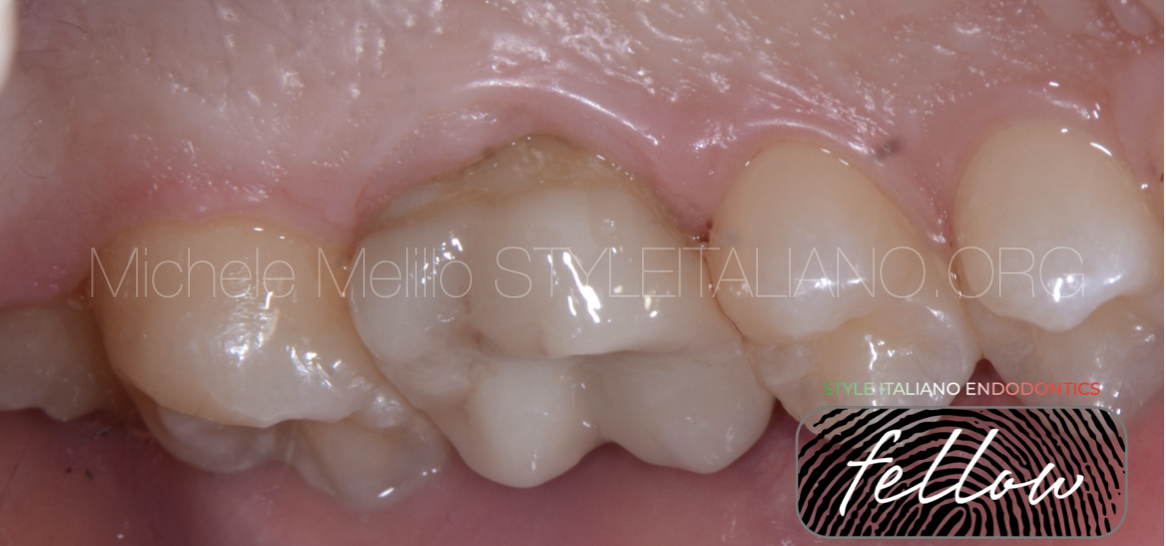
Fig. 12
Confirmed the healing we decided to complete the definitive restoration with an overlay in lithium disilicate.
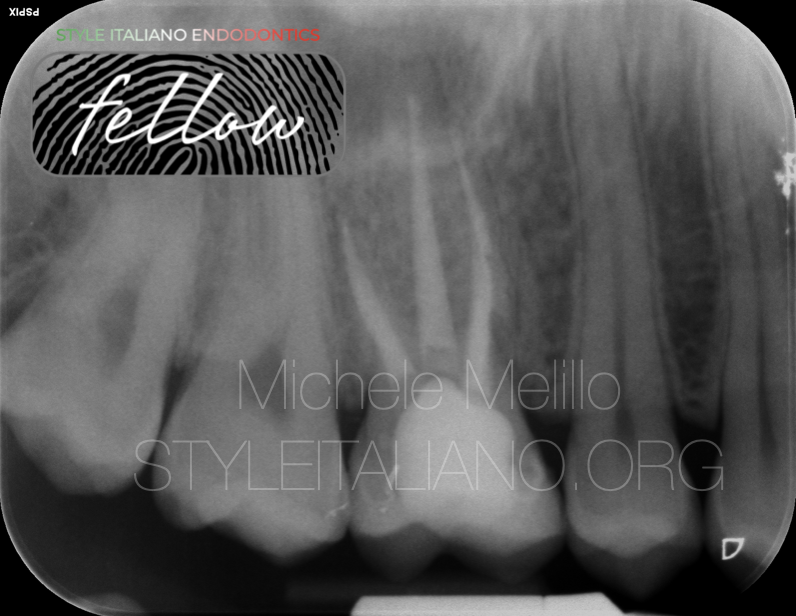
Fig. 13
At 5 years recall the toot is stable, no sings of lesion, no ankylosis.
The patient is satisfied and happy have his tooth still in his mouth.

Fig. 14
About the author:
Michele Melillo
Dr. Michele Melillo graduated with honors in 2009 from University “Politecnica delle Marche”; He is postgraduated in oral surgery from University “G. D’annunzio” in 2016.
Followed several courses in periodontics, implantology and prosthodontics.
His topic of research is on “tooth autotransplantation” and he published some papers about the applications of this technique.
As a clinician he works in his own office in Manfredonia (Puglia, Italy) following complex cases and full mouth rehabilitations.
Dr. Melillo has a teaching collaboration at University of Foggia and gives talks at national and international events on the topics of oral surgery, implant dentistry and prosthodontics.
Conclusions
In case of endodontic lesions, when orthodox approaches are not feasible and when the tooth is considered "lost", the intentional replantation approach should always be considered.
This therapy has simple but strict rules that must be followed rigorously. If respected, the success rate is remarkably high, so high that this solution should be considered much more often. In this clinical case of intentional replantation for root stripping, the 5-year follow-up supports the choice of this path.
Bibliography
Long term survival of mature autotransplanted teeth: A retrospective single center analysis
L. Boschini et al. Journal of Dentistry 98 (2020) 103371
A Systematic Review of the Survival of Teeth Intentionally Replanted with a Modern Technique and Cost-effectiveness Compared with Single-tooth Implants
Anshul Mainkar, DDS, BS J. Endodontics. 2017 Dec;43(12):1963-1968
Intentional Replantation Techniques: A Critical Review
Bradley D. Becker, DDS JOE — Volume 44, Number 1, January 2018

