Fabio Gorni interviews Clifford Ruddle
12/11/2015
The Community
Warning: Undefined variable $post in /home/styleendo/htdocs/styleitaliano-endodontics.org/wp-content/plugins/oxygen/component-framework/components/classes/code-block.class.php(133) : eval()'d code on line 2
Warning: Attempt to read property "ID" on null in /home/styleendo/htdocs/styleitaliano-endodontics.org/wp-content/plugins/oxygen/component-framework/components/classes/code-block.class.php(133) : eval()'d code on line 2
Like the dental extraction, serious endodontic treatment is directed toward removing all the pulp and bacteria, when present, and their related breakdown products from the root canal system.
Clinical treatment steps that comprise start-to-finish endodontics generally include:
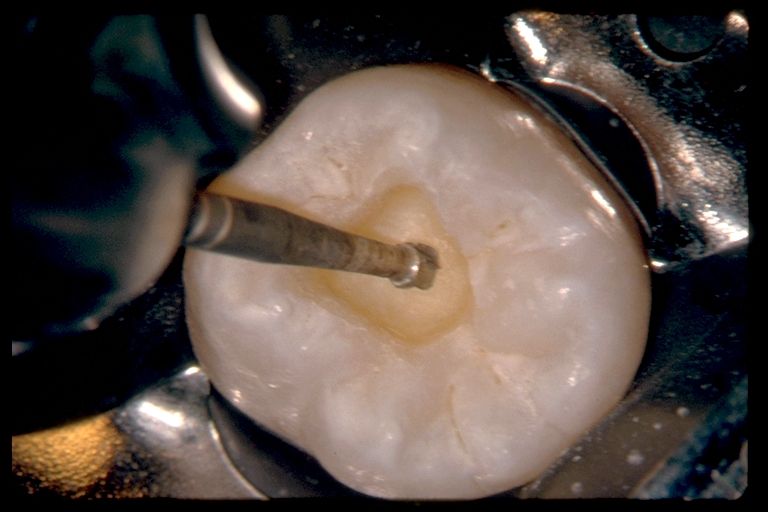
1. Anesthesia, isolation, and cutting the access preparation.
2. Identifying, negotiating, and securing any given canal to its terminal extent. Canals that have been mechanically reproduced and that are secured can be appropriately prepared considering the anatomy of the roots that hold them.
3. Well-shaped canals can be flooded with irrigant. Active irrigation promotes penetration, circulation, and cleaning into all aspects of the endodontic anatomy.
4. Shaping, then, facilitates 3D disinfection and filling root canal systems.
Properly performed, endodontic treatment is the cornerstone of restorative and reconstructive dentistry. Each of these 9 radiographic images demonstrates the importance of clinically negotiating, reproducing, and securing any given canal to its full terminal extent. A secured canal is appropriately shaped to encourage 3D disinfection and filling root canal systems.
Dr. Fabio Gorni interviews Dr. Clifford Ruddle exclusively for Styleitaliano
Fabio: Dear Cliff, it’s been over twenty years since we wrote the script and filmed the video, “The Endodontic Game.” Since then, many things have changed in endo, but do you think that the time-honored or more traditional rationale for treatment is still working? For example, are the crown-down, step-back, or pre-enlargement techniques for preparing canals still winning strategies?
Cliff: Thank you, Fabio. Yes, indeed I have fabulous memories working together with you in Milano 20 years ago. And don’t forget, I was staying in your home the night your baby son was born.
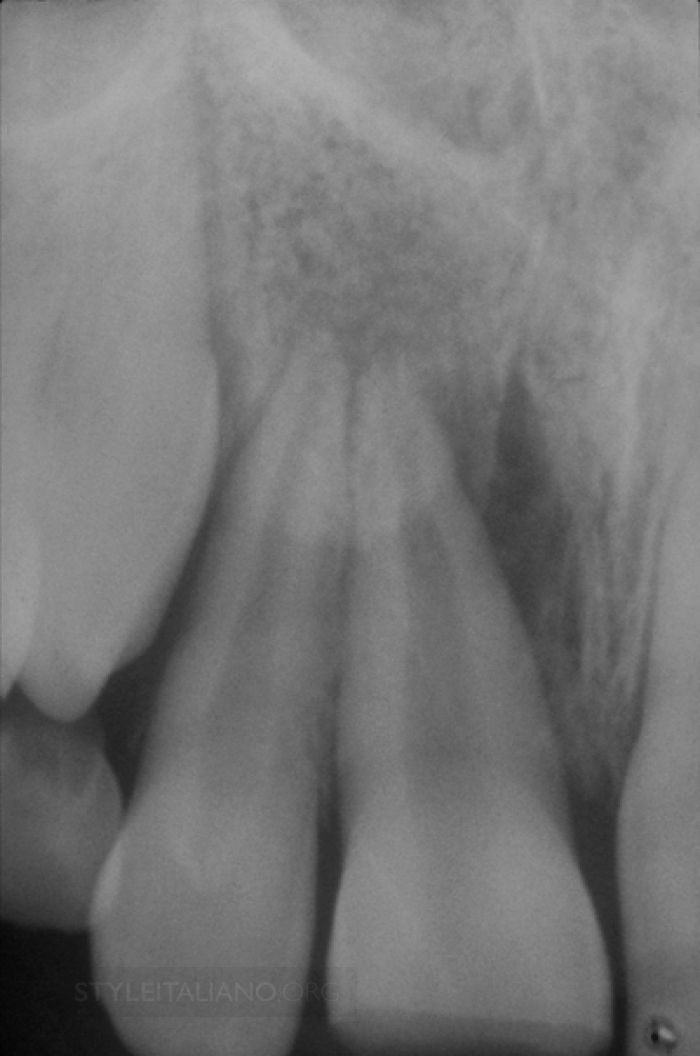
Fig. 1
Regarding your question about the rationale for treatment, I believe that the endodontic rationale for treatment that we outlined in the video series, `The Endodontic Game´, is as relevant today as it was then. While the concepts have endured, it is understandable yes, expected that technology has driven many changes in virtually all clinical procedural steps that comprise start-to-finish endodontics. Regarding the so-called crown-down, step-back, or pre-enlargement techniques each is very different, has been described in different ways, and is intended to promote predictably successful endodontics. Today, clinicians appreciate that first eliminating restrictive dentin from the coronal two-thirds of longer, narrower, and more curved canals is still a winning strategy. Pre-enlargement procedures provide more control and predictability when directing small-sized instruments to the terminus of any given canal.
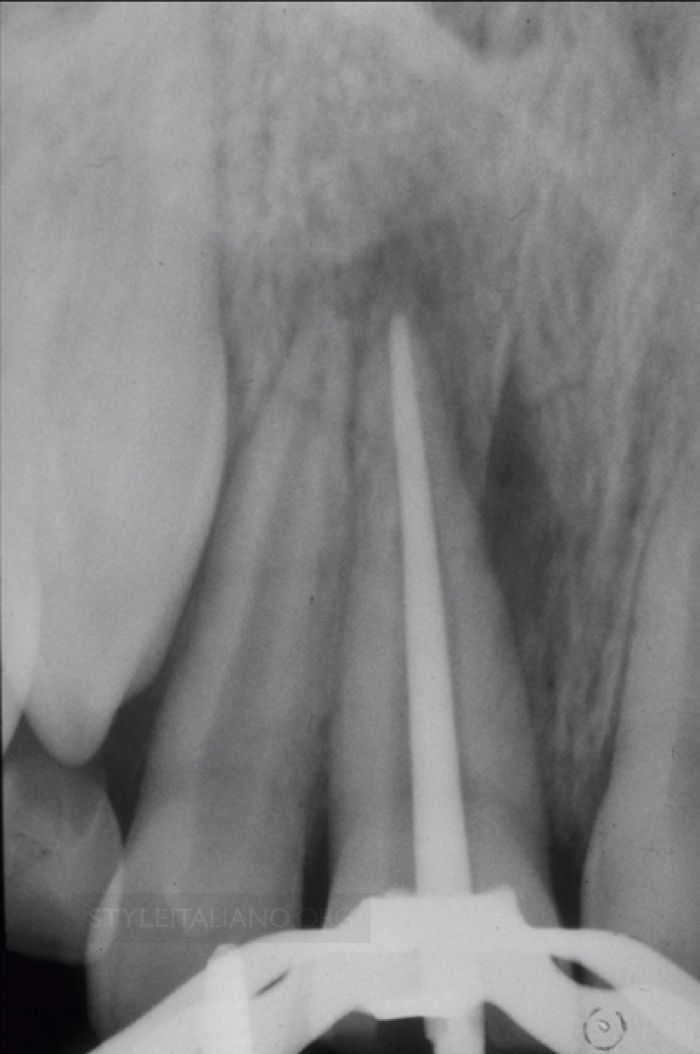
Fig. 2
Fabio: In recent years, some dentists are advocating performing root canal treatment through a very small access cavity. Does size matter?
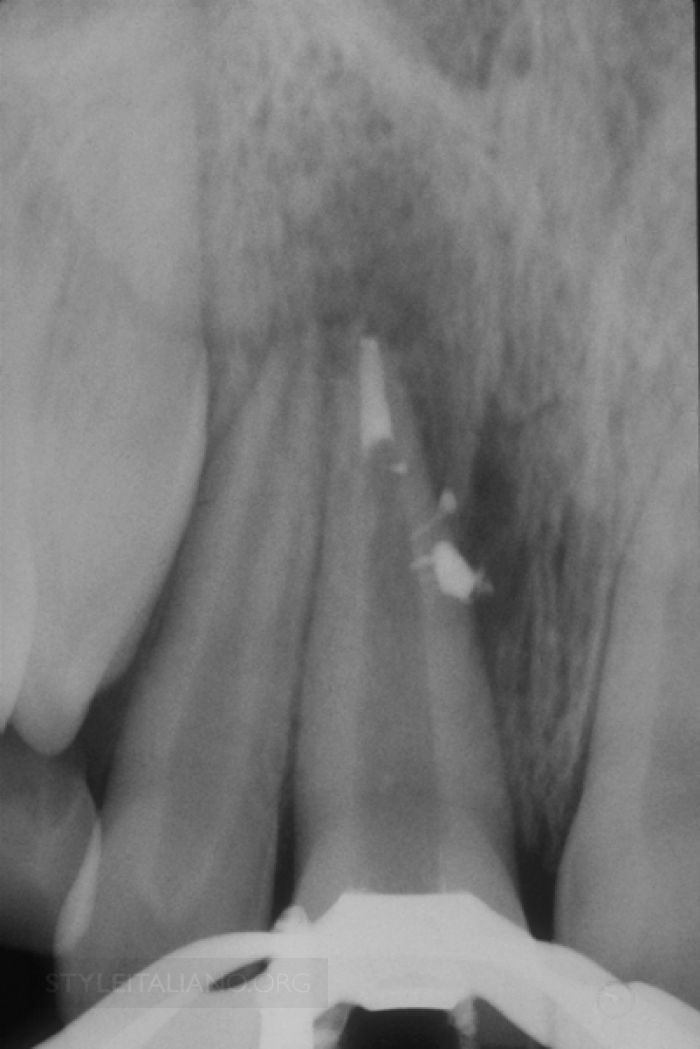
Fig. 3
Cliff: Internationally, and especially in North America, there has been a lot of discussion in the marketplace regarding the size of the access cavity. I became aware of this phenomenon around 2011. During this period, an ultra small group of dentists began promoting the concept of minimally invasive endodontics (MIE). This is a noble concept, as virtually every dentist who performs clinical endodontics wants to maximize and preserve remaining dentin. On the other hand, as a teacher for 41 years, I can report that overly restrictive access cavities commonly lead to missed canals, failure to identify vertical fractures, and tend to compromise the various ensuing steps that serve to guide each case toward a potentially successful conclusion. For example, restrictive access preparations limit the ability to find mid-mesial canals of mandibular molars, MB2s in maxillary molars, or aberrant orifices in any tooth. It is my opinion that restrictive access cavities tend to sabotage success, and for this reason, I do not subscribe to what I consider to be another fad. On the other hand, an access cavity should not be prepared too big, as an over-enlarged access cavity sacrifices tooth structure, weakens teeth, and predisposes to fractures. Ultimately, the size of the access should be driven by the position of the orifices on the pulpal floor of, for example, furcated teeth. The access preparation is deemed finished when the internal axial walls are flared, flattened, and finished.
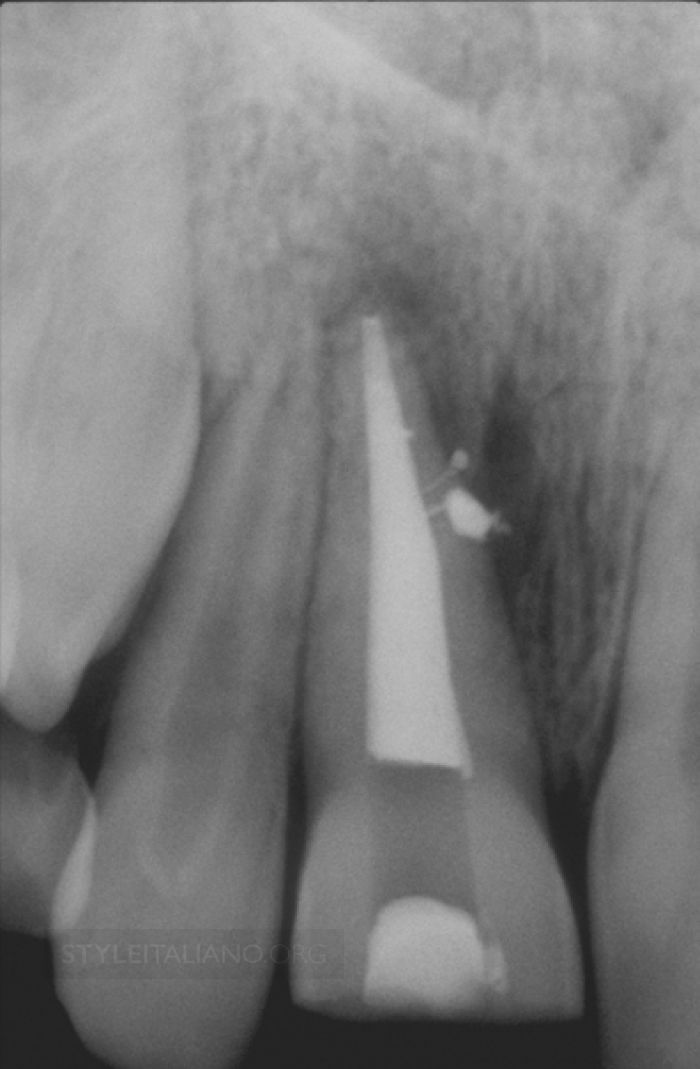
Fig. 4
Fabio: What is your philosophy in endodontics?
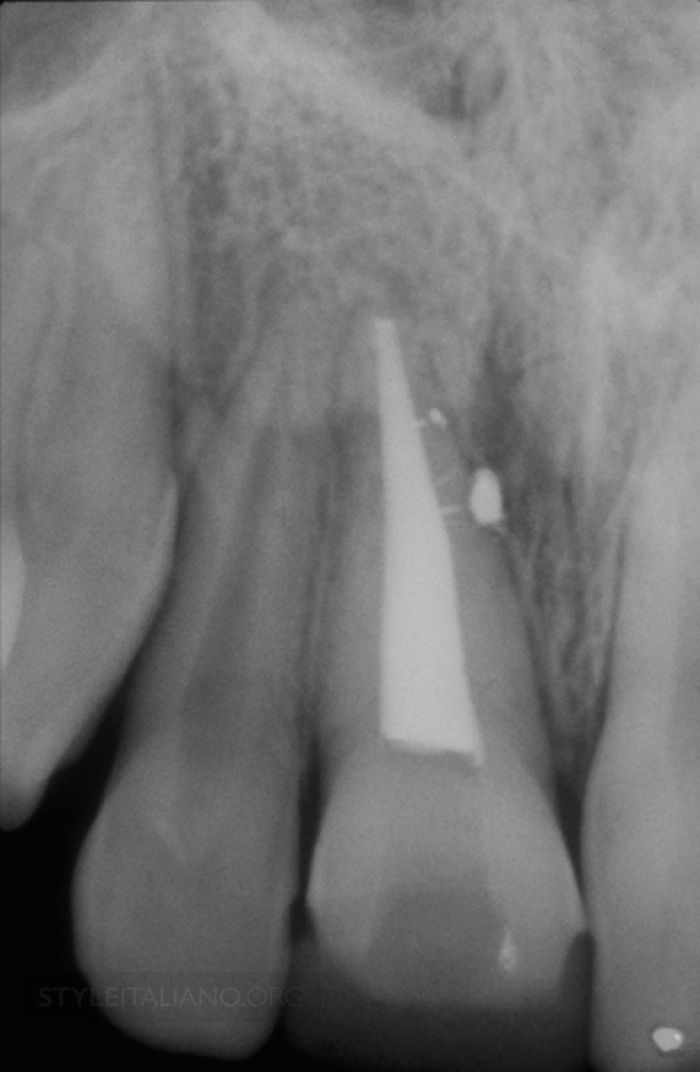
Fig. 5
Cliff: Fabio, you know me pretty well, so I will repeat what I have said for nearly 40 years. My endodontic philosophy parallels the dental extraction. The reason the extraction is successful virtually 100% of the time is related to the fact that the extraction serves to remove all the pulp each time, every time, all the time. Like the extraction, clinical endodontics should be directed toward removing all the pulpal tissue, bacteria when present, and their related breakdown products, while preserving coronal and radicular tooth structure. This is my philosophy of clinical endodontics: to prepare an access cavity that encourages finding orifices, and then to reproduce and prepare these canals to their full working length. Importantly, catheterized, secured, and shaped canals promote 3D disinfection and filling root canal systems.

Fig. 6
Fabio: How do you see the evolution of endodontics today?
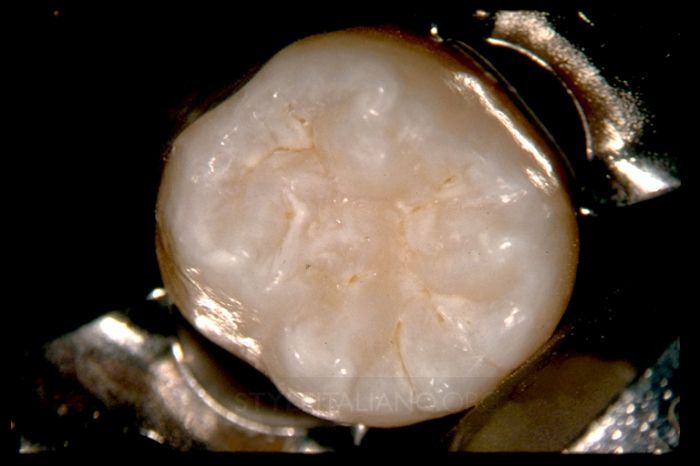
Fig. 7
Cliff: Great question, Fabio, and very exciting. Youve been around endodontics now for, I would imagine, about 25 years, maybe longer, and I think we share the same point of view. The evolution is moving toward reaching the clinical goal for endodontics: namely, complete disinfection.
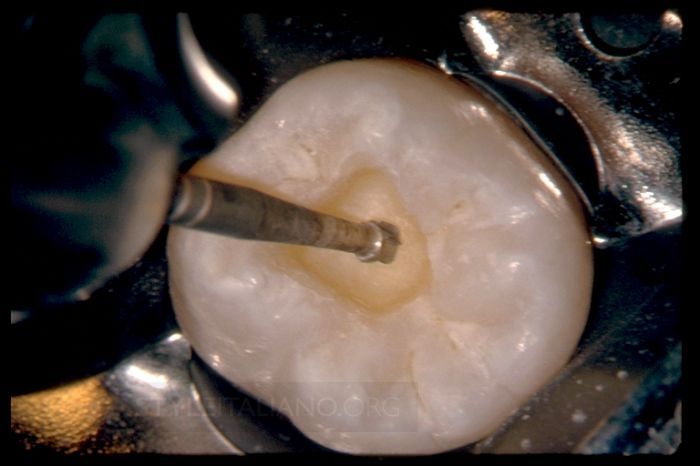
Fig. 8
Looking at disinfection, there is relentless focus on ways to improve the exchange of reagents. Various groups are using mechanical, light, or sound methods to improve fluid dynamics. Further, improvements are coming with the reagents, themselves. For example, a specific light-activated reagent can release singlet oxygen, which in turn, can implode and kill bacteria. Yet, with all this promise, the Holy Grail of disinfection is any given method must have collaborative evidence, be easy to use, and be readily affordable. At this time, that product is the EndoActivator, which is heavily supported by peer-reviewed scientific evidence and used daily by over 35,000 dentists. Regarding obturation, as we improve on our cleaning, we can absolutely begin to fulfill the future promise of a biologically improved obturation material. These materials can be designed as a scaffold to hold both a sealer and cone together. The material does not necessarily have to be gutta percha, but the promise is, we can approach sealing clean root canal systems using innovative new materials that encourage bone growth, and are biocompatible, dimensionally stable, and biologically inert. So we will see vast improvement in both materials and the delivery systems for both fully vs. minimally prepared canals. nnThere is a dental technology company called Healthdent, located in Southern California and owned by a practicing dentist, Dr. Nathan Lee. He has invented a new manufacturing method to make gutta percha master cones (GPMCs) that have tolerances within machining tolerances. This means, if you are using system-based endodontics, when you remove the last working file to length, the correspondingly-sized GPMC will precisely fit this shape. Healthdent has rapidly become the industry leader in GPMC sizing. Equally important, Healthdent has improved gutta percha formulation through nanotechnology. This specific technology has resulted in a 2-3 mm extended heat wave through the GPMC upon thermosoftening, as compared to all other competitive cones. Recall, Schilder first described the vertical condensation of warm gutta percha in 1967. So, Healthdent is fulfilling Schilder´s vision for predictable and effective obturation with its new GPMC that has better sizing, improved formulation, and is latex free. In Europe, these master cones are being sold through Charles B. Shwed and, more limited, through Dentsply Endodontics or Maillefer. In North America, Charles B. Schwed and Dentsply Tulsa Dental Specialties already have system-based cones for ProTaper Gold and WaveOne Gold, for example.
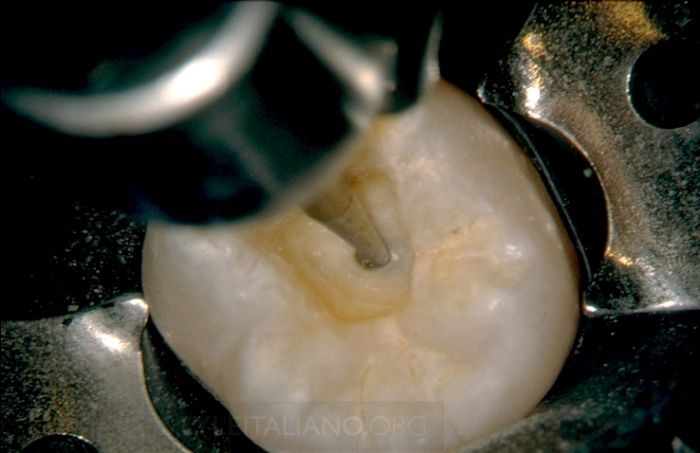
Fig. 9
Fabio: You are a leading expert in clinical endodontics. From where do you get your inspiration?
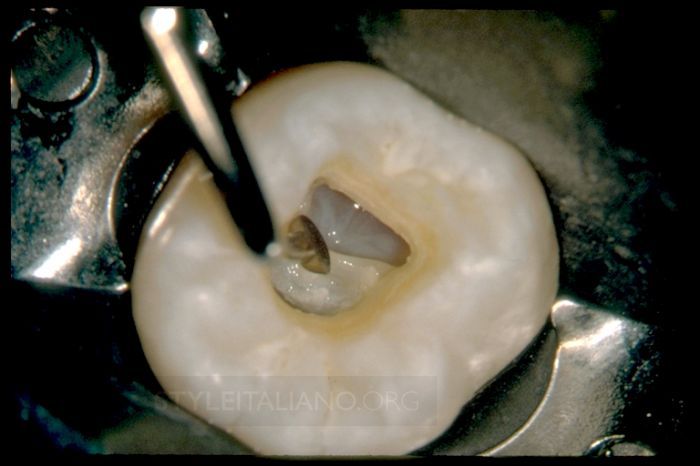
Fig. 10
Cliff: This is an easy question. My father and mother were fantastic role models who most influenced me and taught me life´s great lessons. I was taught that inspiration is found through hard work, focus, and perseverance. These traits or characteristics definitely apply to endodontics. In the world of endodontics, my interest as a dental student was first kindled by Dr. Ron Borer at the University of the Pacific in San Francisco. As a post-grad endo student at Harvard School of Dental Medicine, my mentor, Dr. Alvin Arlen Krakow, really ignited this fire within me and gave me a vision of what endodontics could be when properly performed. During this period, Prof. Herbert Schilder created the endodontic inferno that passionately burns inside me to this moment. Fabio, I do not want to embarrass you, but you have influenced me because, even though you are my contemporary and considerably younger than me, I have learned a great deal from having watched you work. Certainly, I have learned from Gary Carr, Steve Buchanan, Pierre Machtou, John West, and Tom McClammy, to name a few. I have learned from so many, but this is most important, it´s my family, friends, and colleagues who empower me, inspire me, and encourage me to be the best I can be.
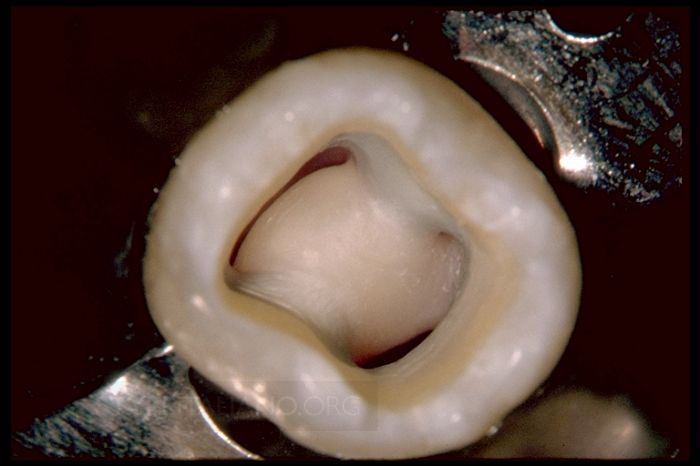
Fig. 11
Fabio: You are admired for being a superb teacher. What is your attitude about sharing your knowledge?
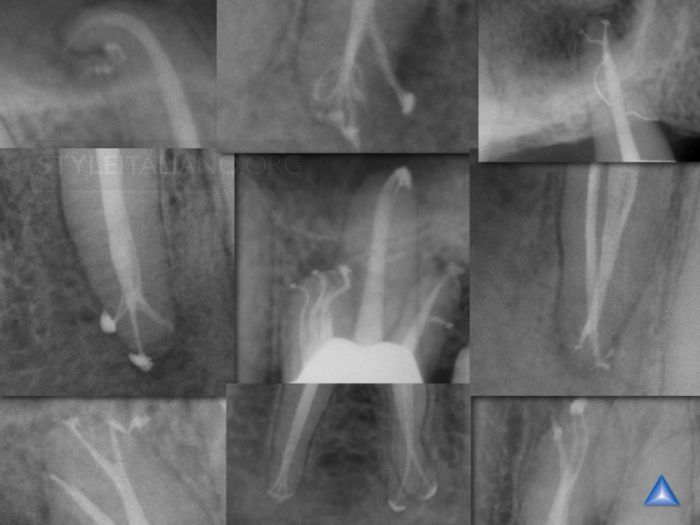
Fig. 12
Cliff: I will go back to my pop. Pop used to say, ``you cannot antagonize and influence at the same time.´´ It is essential to teach basics, develop talent, and spark the greatness that virtually every human has locked inside them. Genuine teachers want their students to go beyond them. I believe we can disagree, yet remain kind, even when there is a strong disagreement. As I get older, it´s less important to be right; it is most important to me to make people around me more successful. So I believe we teach, demonstrate, and inspire our students. We must give students a learning environment that is comfortable, safe, and fun, and also that fosters confidence, growth, and moves them closer toward their full potential.
